The hidden challenge to quality care
Team
Communication
Our lab focuses on the various communication processes in surgical care, both between children, families/caregivers and their providers, and within interprofessional care teams.

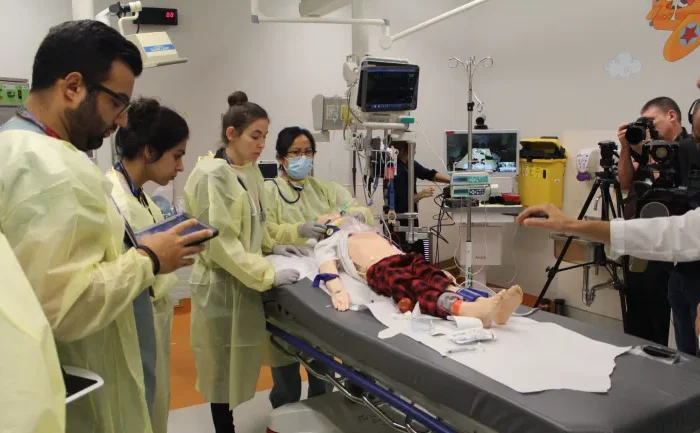
Health sciences education is complex and unique, requiring expertise across multiple domains. Students are required to learn not only vast amounts of knowledge and technical procedures but also to acquire key communication and other non-technical skills, including leadership, situational awareness, decision-making, and teamwork. Such skills are essential for teams to manage critical situations effectively and efficiently. Indeed, poor communication within teams contributes to most healthcare errors, and these vital skills are best taught through simulated scenarios.
Despite the documented importance of non-technical skills training, curricula incorporating them in healthcare settings are notably absent, particularly in surgical education. In a recent review of Canadian teaching hospitals, objectives for non-technical skills learning were only considered in 0.76% of surgical interventions. Although the importance of non-technical skills is generally recognized, there remains a gap in teaching modalities to help the students and trainees acquire these skills. We intend to fill this gap by formally formally teaching non-technical skills to students and trainees through simulation, using standardized instructional and evaluative tools.
Our other over-arching objective for simulation training is to leapfrog it decisively into the 21st century, by replacing physical mannequins (high- or low-fidelity) with immersive virtual and mixed reality environments. We aim to do this first in the context of pediatric trauma, though it is applicable to a variety of clinical and education simulation environments. At a time when all simulation in other scientific domains is accomplished virtually, it’s about time we caught on with this in medicine!